We asked Prof. James Spratt and Dr. Simon Wilson to share their IVL journey since the launch of Shockwave C2 five years ago and their initial experience with the new Shockwave C2+. Regardless of the physicians experience, the overall opinion is the same: “IVL is quick to learn, easy to use, very safe, and effective across a broad range of calcium types that other technologies can’t compete with. It has changed the landscape for calcium modification and the new Shockwave C2+ catheter continues to expand physicians ability to deal effectively and safely with severe calcium in a broader range of patients.” Read more below:
Shockwave Medical launched its coronary catheter, Shockwave C2, five years ago and you were one of the first consultants using IVL. Can you take us back to the beginning to the first time you used it and what your thoughts were?
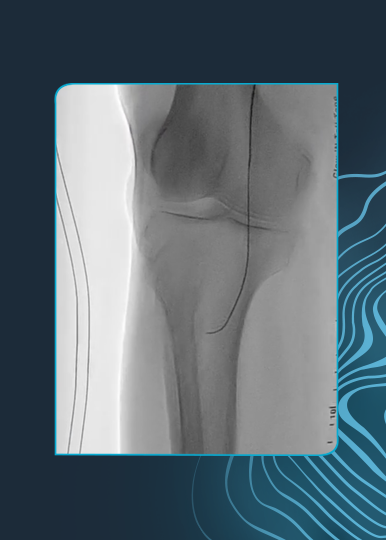
Prof. Spratt: With the initial launch, we were very curious to understand whether the product worked! Often where there is hype, it is swiftly followed by disappointment, but not in this case. Instrumental to our understanding of how and where IVL worked was our use of intravascular imaging. It was highly instructive to see fractures in previously rigid calcium and highly rewarding to get excellent results in challenging patients. Yet, despite the impressive efficacy, the safety profile is what reassured us to continue to explore what IVL could offer.
Your generation was once referred to as the “IVL generation.” Can you tell us about your experience with coronary intravascular lithotripsy (IVL) and how it influenced and shaped your treatment algorithm for calcified lesions?
Dr. Wilson: I was a keen user of atherectomy but quite often felt a bit disappointed with the outcome and never felt that cutting or high-pressure balloons were remotely suited to dealing with severe calcium. IVL has been hugely impactful to my practice. It is so easy to use, extremely safe, and just makes sense in terms of the mechanism of action. There is no doubt that having IVL available has allowed me to treat a much wider range of calcium types in a broader range of patients with a high degree of confidence in the devices safety and the final result.
How did IVL change your approach to the treatment of calcified lesions? Can you comment on your contemporary calcium algorithm compared to five years ago when IVL was introduced?
Prof. Spratt: Prior to the introduction of IVL, the options for treating patients with severe calcified coronary artery disease (CCAD) were limited. We frequently used rotational atherectomy and indeed continue to do so, but were aware of its limitations in failing to address deep calcium or indeed performing significant debulking. Following rota, all the other options were balloon-based, with the attendant limitations in nodular or eccentric calcium. This led to safety concerns over high-pressure balloon inflation & the risks of vessel perforation and ultimately led to less good clinical outcomes for patients. It is fair to say that IVL changed this landscape fundamentally & is now the treatment of choice for virtually all types of CCAD. Rotational atherectomy remains the treatment of choice for critical or uncrossable lesions, but beyond this, if the calcium burden is significant, IVL is the therapy of choice.
How would you describe the mechanism of action of IVL to your colleagues that are just starting with IVL? How does it compare with other specialty balloons?
Dr. Wilson: Non-compliant, cutting, and OPN balloons all work through applying hydrostatic force and are therefore not selective for calcium. On inflation, they will invariably expand away from resistance and with high-pressure inflations, risk major barotrauma. IVL as we know uses shockwaves that travel through the vessel wall generating disruptive forces only when calcium is encountered. IVL is therefore selective for calcium and can modify both superficial and deeper calcium as well as eccentric, concentric and nodular sub-types. Where there is significant calcium that has not resolved with an NC balloon at standard pressures, I no longer see an obvious role for anything other than IVL or atherectomy.
As one of the leading IVL centers in Europe, you had the chance to test first-hand the new Shockwave C2+ catheter with 50% more pulses. In general, what are your impressions of Shockwave C2+?
Prof. Spratt: We have been pleased. It extends the possibilities of IVL, enabling us to target more challenging lesions, such as nodular calcium, or longer lesions. There appears to be no durability or safety trade-off, so the access to 50% more “shocks” for the same cost is a win-win.
What case types or patient types that you believe the new Shockwave C2+ can better address compared to Shockwave C2?
Dr. Wilson: Broadly speaking, the impact of balloons relates to the hydrostatic force applied. Atherectomy depends on the contact area, whereas IVL can be thought of in terms of energy (or pulses) applied. The 50% increase in pulses gives you the confidence to deal with longer segments of severe calcium or two vessel calcific disease, where previously you might be reaching for atherectomy. I also find the extra pulses can be especially useful in thick eccentric calcium, as we know this type of calcium can often need a bit more energy to resolve.
Do you have any tips to share with people who are just starting to use IVL, particularly for the new catheter with 120 pulses?
Prof. Spratt: The first “tip” is to watch the Shockwave Calcium Masterclass series! This will provide a solid understanding of both the technology and lesion understanding. As with any technology, understanding the goals of therapy, in this case restoration of vessel compliance sufficient to allow full stent expansion, is critical. To properly integrate IVL into your practice, intravascular imaging is essential. The Masterclass Series, produced in partnership with Optima Education is foundational in this respect and highly recommended.
Can you explain what “pulse management” with IVL means and how do you think about applying pulses when you’re treating different types of calcium morphologies? Will your pulse management strategies change with 120 pulses?
Dr. Wilson: To get the most out of IVL, it’s important to focus therapy on the most resistant segments. If it is a short segment of calcific disease, then it’s easy – put all the energy into that one spot. However, it’s very common to be dealing with much longer segments of calcific disease and although the C2+ gives you more margin, it’s still important to concentrate the majority of pulses into the most resistant segment or segments. I therefore make sure to understand where the most severe calcium on imaging is located angiographically and I almost always attempt pre-dilatation with a standard balloon ahead of IVL to understand where the greatest resistance is. Armed with this knowledge I then work from distal to proximal, covering the entire calcific segment with IVL but focusing the majority of pulses into the most resistant segments.
Will your calcium algorithm change with the introduction of Shockwave C2+? If so, can you take us through the changes?
Prof. Spratt: The most obvious iteration will be the ability to address longer sections of disease, or by targeting nodular or eccentric calcium. Important questions remain around what is the threshold of calcium that requires IVL; how best to identify an effective response, especially in nodular calcium and pulse management. We remain excited to explore these questions through research and education, what this space!
Drs. Spratt and Wilson are paid consultants for Shockwave Medical.
Coronary Important Safety Information:
In the United States: Rx only.
Indications for Use—The Shockwave Intravascular Lithotripsy (IVL) System with the Shockwave C2 Coronary IVL Catheter is indicated for lithotripsy-enabled, low-pressure balloon dilatation of severely calcified, stenotic de novo coronary arteries prior to stenting.
Contraindications—The Shockwave C2 Coronary IVL System is contraindicated for the following: This device is not intended for stent delivery. This device is not intended for use in carotid or cerebrovascular arteries.
Warnings— Use the IVL Generator in accordance with recommended settings as stated in the Operator’s Manual. The risk of a dissection or perforation is increased in severely calcified lesions undergoing percutaneous treatment, including IVL. Appropriate provisional interventions should be readily available. Balloon loss of pressure was associated with a numerical increase in dissection which was not statistically significant and was not associated with MACE. Analysis indicates calcium length is a predictor of dissection and balloon loss of pressure. IVL generates mechanical pulses which may cause atrial or ventricular capture in bradycardic patients. In patients with implantable pacemakers and defibrillators, the asynchronous capture may interact with the sensing capabilities. Monitoring of the electrocardiographic rhythm and continuous arterial pressure during IVL treatment is required. In the event of clinically significant hemodynamic effects, temporarily cease delivery of IVL therapy.
Precautions— Only to be used by physicians trained in angiography and intravascular coronary procedures. Use only the recommended balloon inflation medium. Hydrophilic coating to be wet only with normal saline or water and care must be taken with sharp objects to avoid damage to the hydrophilic coating. Appropriate anticoagulant therapy should be administered by the physician. Precaution should be taken when treating patients with previous stenting within 5mm of target lesion.
Potential adverse effects consistent with standard based cardiac interventions include– Abrupt vessel closure – Allergic reaction to contrast medium, anticoagulant and/or antithrombotic therapy-Aneurysm-Arrhythmia-Arteriovenous fistula-Bleeding complications-Cardiac tamponade or pericardial effusion-Cardiopulmonary arrest-Cerebrovascular accident (CVA)-Coronary artery/vessel occlusion, perforation, rupture or dissection-Coronary artery spasm-Death-Emboli (air, tissue, thrombus or atherosclerotic emboli)-Emergency or non-emergency coronary artery bypass surgery-Emergency or non-emergency percutaneous coronary intervention-Entry site complications-Fracture of the guide wire or failure/malfunction of any component of the device that may or may not lead to device embolism, dissection, serious injury or surgical intervention-Hematoma at the vascular access site(s)-Hemorrhage-Hypertension/Hypotension-Infection/sepsis/fever-Myocardial Infarction-Myocardial Ischemia or unstable angina-Pain-Peripheral Ischemia-Pseudoaneurysm-Renal failure/insufficiency-Restenosis of the treated coronary artery leading to revascularization-Shock/pulmonary edema-Slow flow, no reflow, or abrupt closure of coronary artery-Stroke-Thrombus-Vessel closure, abrupt-Vessel injury requiring surgical repair-Vessel dissection, perforation, rupture, or spasm.
Risks identified as related to the device and its use: Allergic/immunologic reaction to the catheter material(s) or coating-Device malfunction, failure, or balloon loss of pressure leading to device embolism, dissection, serious injury or surgical intervention-Atrial or ventricular extrasystole-Atrial or ventricular capture.
Prior to use, please reference the Instructions for Use for more information on warnings, precautions and adverse events. https://shockwavemedical.com/IFU
Please contact your local Shockwave representative for specific country availability and refer to the Shockwave C2 instructions for use containing important safety information.