Moving Calcium Modification Forward: Shockwave Javelin Case Review
Shockwave Javelin helps expand your treatment options across calcified peripheral lesions. Dr. Charles Bailey, Emory University Hospital, used Shockwave Javelin in the anterior tibial (AT), dorsalis pedis (DP) and pedal-plantar loop of a 67-year-old male patient suffering from left foot nocturnal rest pain and a recurrent toe ulceration. His medical history included diabetes mellitus, hypertension, congestive heart failure and a prior femoral-to-proximal AT prosthetic bypass graft. Revascularization goals included improved forefoot perfusion and improved outflow tract for long-term graft durability.
-
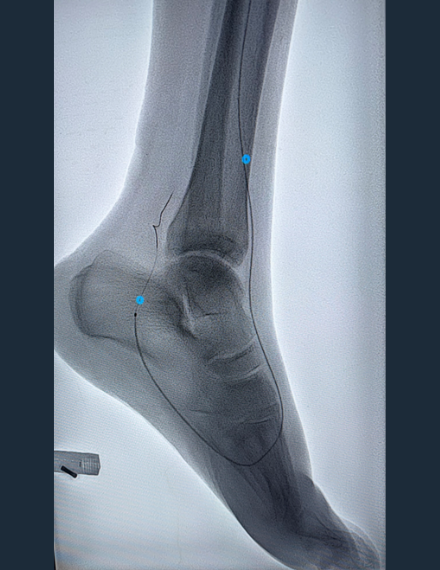
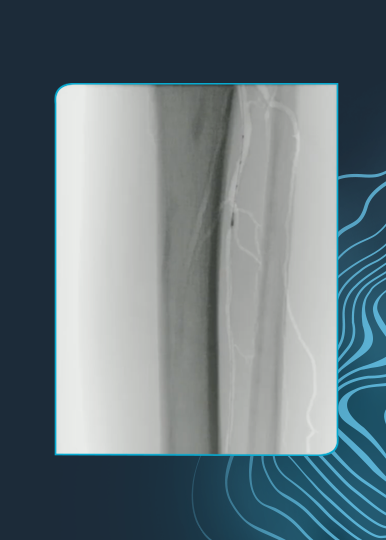
Pre-Procedure Angio
 Occlusive calcium in AT extending into DP
Occlusive calcium in AT extending into DP -
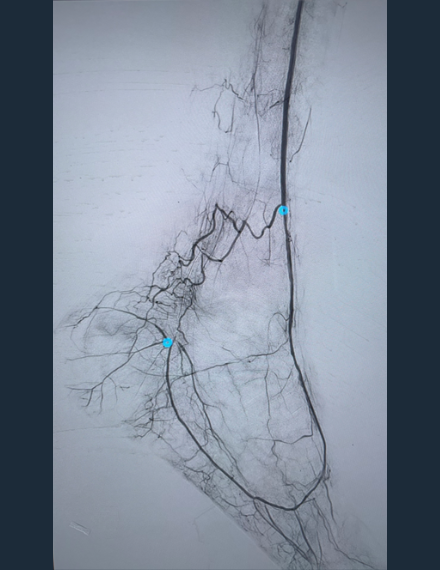
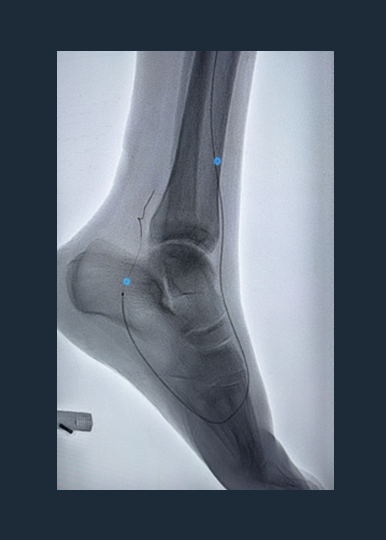
Shockwave Javelin Treatment Angio
 120 pulses delivered across occlusive segments
120 pulses delivered across occlusive segments -
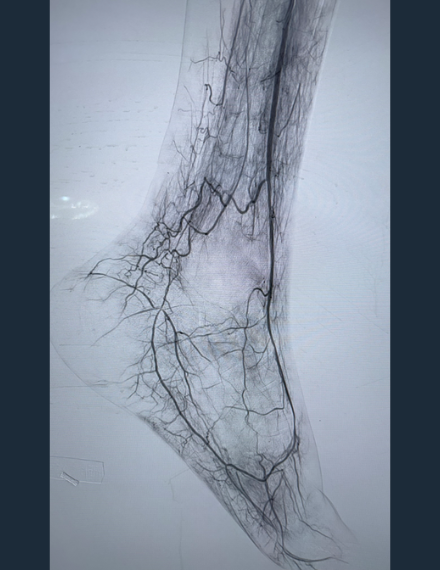
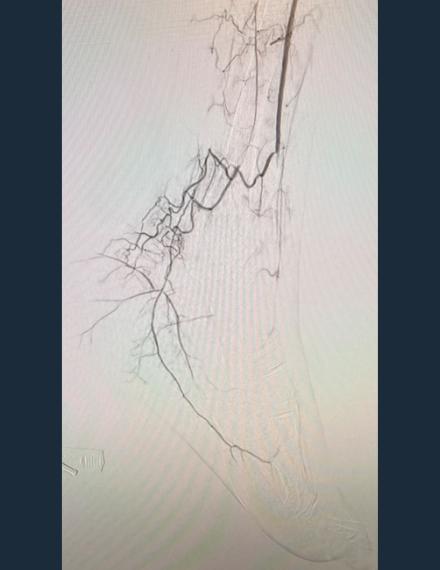
Post-Shockwave Javelin Angio
 Restored patency to distal AT, DP and pedal-plantar loop
Restored patency to distal AT, DP and pedal-plantar loop -
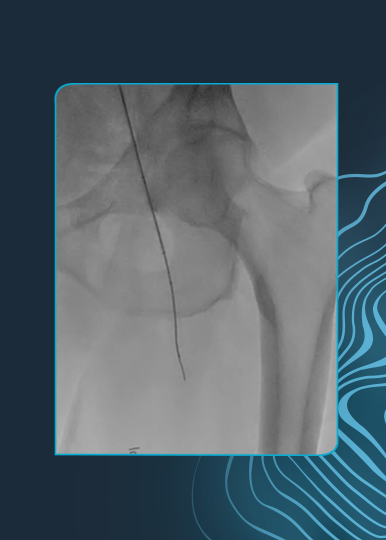
Final Angio
 Brisk flow restored throughout treated vasculature
Brisk flow restored throughout treated vasculature
Learn more about Shockwave Javelin
Procedural Details
Pre-procedural vascular testing showed absent great-toe pressure, occlusion of the distal anterior tibial and dorsal pedal arteries, and a patent but low-velocity bypass graft with poor distal outflow consistent with chronic limb-threatening ischemia. The distal AT and DP lesions were traversed intraluminal and Shockwave Javelin was used to modify the heavily calcified plaque followed by a percutaneous transluminal angioplasty (PTA) balloon.
Peri-procedural management included systemic heparinization with activated clotting time (ACT) >> 250 seconds and use of low-profile crossing and support catheters to protect the bypass while optimizing outflow to improve graft-assisted patency.
Post-operatively, Dr. Bailey continues to monitor the patient’s restored distal perfusion, wound healing and graft patency while optimizing medical comorbidities to preserve limb salvage and long-term graft durability.
Pre-op Vascular Lab Testing
No great toe pressure; dorsal pedal occlusion.
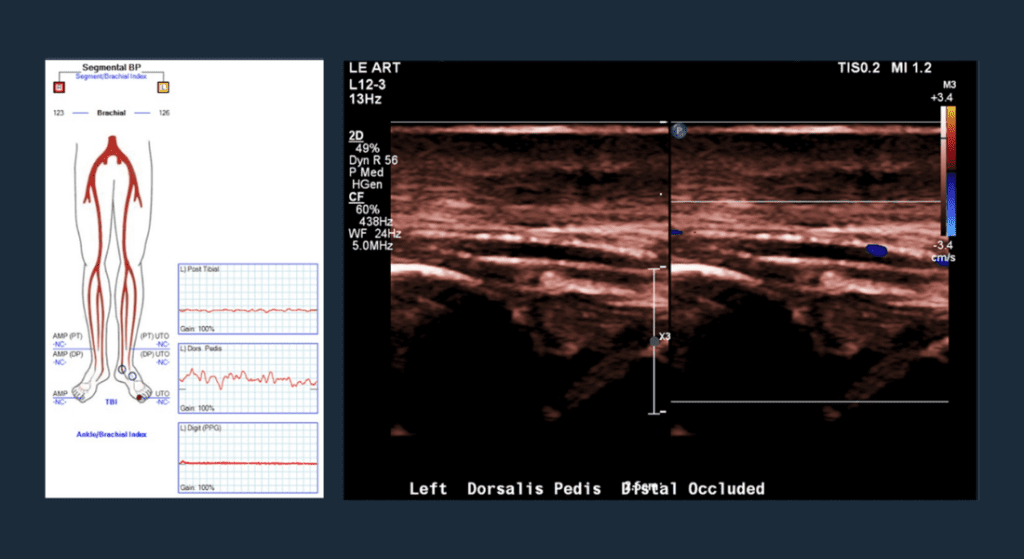
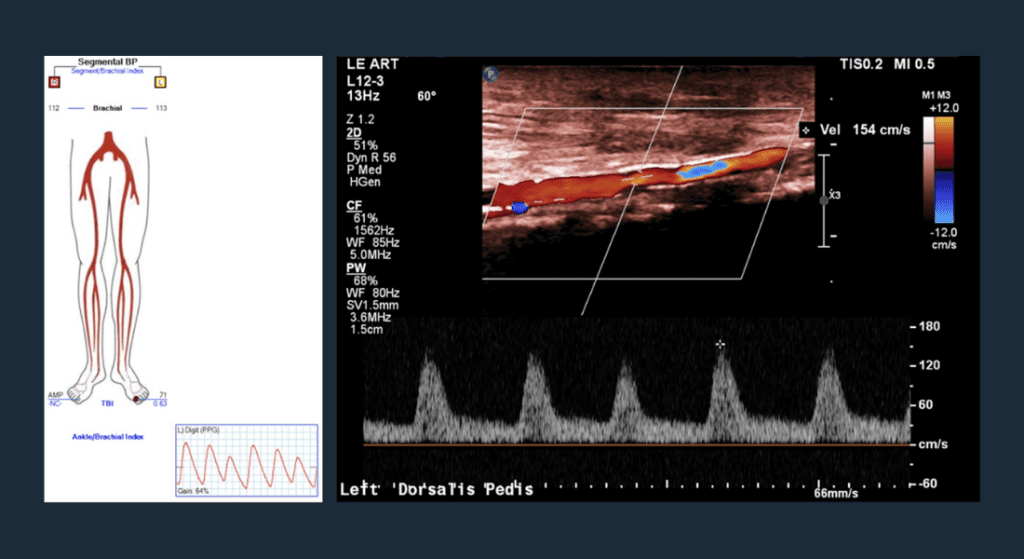
Post-op Vascular Lab Testing
Great toe pressure restored to 71mmhg; widely patent dorsal pedal vessel.
Dr. Bailey is a paid consultant of Shockwave Medical.
Shockwave IVL: In the U.S.: Rx only. Prior to use, please reference the Important Safety Information for more information on indications, contraindications, warnings, precautions and adverse events.